Page 15 / March 07
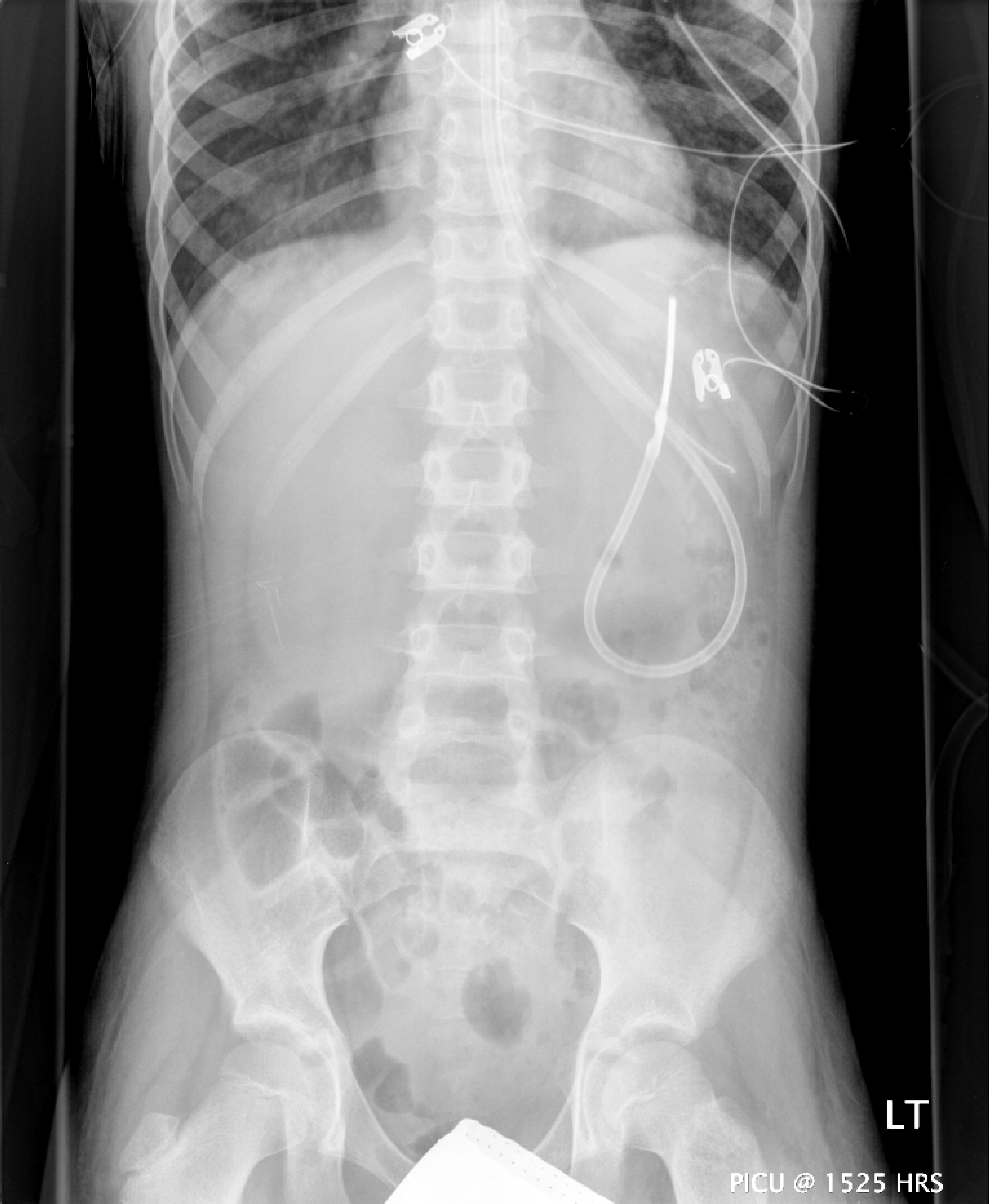 He was not bronchoscoped as there was a repeat X-ray at midday showing significant re-aeration of the right middle and lower lobes. atelectasis had resolved.
However, he continued to have persistently high oxygen and ventilatory requirement. 2 days later he desaturated to the low 70's and could not be oxygenated. A bronchoscopy by the intensivist was not only diagnostic in identifying a right bronchial cast, but was also therapeutic with the removal of this cast and blood clots resulting in significant clinical improvement and saturations rising to 95%.
He was not bronchoscoped as there was a repeat X-ray at midday showing significant re-aeration of the right middle and lower lobes. atelectasis had resolved.
However, he continued to have persistently high oxygen and ventilatory requirement. 2 days later he desaturated to the low 70's and could not be oxygenated. A bronchoscopy by the intensivist was not only diagnostic in identifying a right bronchial cast, but was also therapeutic with the removal of this cast and blood clots resulting in significant clinical improvement and saturations rising to 95%.
By day 25 he stopped bleeding and his ventilatory requirements steadily came down with an FiO2 on day 26 of admission of only 0.35 and settings of 13/5. He was noted to have peripheral and proximal muscle weakness, probably secondary to the continuous methlprednisolone. He was extubated on day 28 of admission and the methylprednisolone was reduced to 2 mg/kg/day. His CXR had cleared.
On the ward he was initially mentally disturbed with post ICU delusion. He contracted two proven urinary tract infections. He also had to be maintained on anti-hypertensive medication at the beginning secondary to steroid treatment.
Soon after transfer he was switched onto oral prednisolone at 2 mg/kg/day. This dose was reduced prior to discharge with the plan to wean it down further. He had regular physiotherapy and by day 41 he was walking with gradual increase in his muscle strength.
He had his lung function prior to discharge. His FEV1 was 67% and post bronchodilator it was 80%. His FVC was 60% and Total Lung Capacity 71%. His residual lung volume over TLC was 29%. The DLCO was 75%.
 Next page /
Next page /
ANSWER:
 He was not bronchoscoped as there was a repeat X-ray at midday showing significant re-aeration of the right middle and lower lobes. atelectasis had resolved.
However, he continued to have persistently high oxygen and ventilatory requirement. 2 days later he desaturated to the low 70's and could not be oxygenated. A bronchoscopy by the intensivist was not only diagnostic in identifying a right bronchial cast, but was also therapeutic with the removal of this cast and blood clots resulting in significant clinical improvement and saturations rising to 95%.
He was not bronchoscoped as there was a repeat X-ray at midday showing significant re-aeration of the right middle and lower lobes. atelectasis had resolved.
However, he continued to have persistently high oxygen and ventilatory requirement. 2 days later he desaturated to the low 70's and could not be oxygenated. A bronchoscopy by the intensivist was not only diagnostic in identifying a right bronchial cast, but was also therapeutic with the removal of this cast and blood clots resulting in significant clinical improvement and saturations rising to 95%.By day 25 he stopped bleeding and his ventilatory requirements steadily came down with an FiO2 on day 26 of admission of only 0.35 and settings of 13/5. He was noted to have peripheral and proximal muscle weakness, probably secondary to the continuous methlprednisolone. He was extubated on day 28 of admission and the methylprednisolone was reduced to 2 mg/kg/day. His CXR had cleared.
On the ward he was initially mentally disturbed with post ICU delusion. He contracted two proven urinary tract infections. He also had to be maintained on anti-hypertensive medication at the beginning secondary to steroid treatment.
Soon after transfer he was switched onto oral prednisolone at 2 mg/kg/day. This dose was reduced prior to discharge with the plan to wean it down further. He had regular physiotherapy and by day 41 he was walking with gradual increase in his muscle strength.
He had his lung function prior to discharge. His FEV1 was 67% and post bronchodilator it was 80%. His FVC was 60% and Total Lung Capacity 71%. His residual lung volume over TLC was 29%. The DLCO was 75%.
