PRESENTING FELLOW
Tareq Al-Abdoulsalam,
respiratory resident,
Montreal Children's Hospital.
Introduction
A 3-year old boy, who was previously healthy, presented to the emergency department at Montreal Children’s Hospital with fever and cough for 2 weeks.
History
Prior to his presentation, he had a 2-week history of undocumented fever (he felt warm to touch). This was associated with a cough that was insidious in onset, and described as wet with no diurnal variation. There was no history of chocking or foreign body aspiration.
A review of systems showed that he had coryza, but no history of other respiratory symptoms, no sick contacts, no constitutional symptoms, and no recent travel outside Canada.
Pregnancy was uneventful, and delivery was at term. Past history was non contributory. Immunizations were up to date, and the patient was not receiving regular medications.
Family history was negative for respiratory illness or atopy.
Physical Examination
In the emergency department, the patient’s vital signs were stable: he was afebrile (temperature: 36.5oC), not tachypneic (RR: 26/min), and the SaO2 at room air was normal (95%). The chest exam showed decreased breath sounds in left hemithorax. The rest of physical examination was unremarkable.
Investigations
At that point, the working diagnosis in the emergency department was to rule out pneumonia. A complete blood count and blood culture were done and both results were normal.
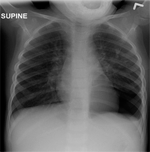
A chest radiograph was done. After reviewing the findings on that X-ray film, the pulmonary service was consulted.