ANSWER:
We did the following:
Bronchoscopy and broncheoalveolar lavage.
PPD planted.
CT Scan not performed at this time.
The bronchoscopy revealed a friable mucosa throughout, especially in the right lower lobe and thick white secretions in the left lower lobe.
The PPD was 0 mm.
The broncheoalveolar samples revealed a gram stain with over 25 WBC/high powered field and less than 10 epithelial cells. No bacteria were seen. Cultures were negative for bacteria, fungus and tuberculosis. No acid fast bacilli were seen on the smear and tuberculosis PCR was negative. Viral cultures were negative. On the pathology slides of the BAL there was no PCP, no cellular changes or viral inclusions and evidence of a mild acute and chronic inflammation seen.
At this point the patients treatment included IV Septra (initially 20mg/kg/day of trimethaprim which was subsequently changed to a prophylaxis dose after results of the lavage), IV Vancomycin and IV Piperacillin/Tazocillin. The patient was also on IV Acyclovir (positive Herpes simplex virus oral culture) and IV Amphotericin B (positive Candida oral culture and evidence of esophagitis on upper endoscopy). Over the 7 days she developed multi-organ failure including acute renal failure requiring dialysis, hypotension requiring inotrope support, an upper gaatro-intestinal bleed, liver failure with coagulopathy, hypothermia (T-32.5ºC) and pancreatitis.
As of day 15, the positive investigations included confirmation of HIV positive status with a CD4 count of 6, S. Aureus positive blood culture (Day 6), Candida positive esophagitis and a Herpes Simple -1 Virus positive esophagitis.
Her treatments included IV Meropenem and IV Amikacin (started after worsening of status on Day 15), IV Vancomycin (continued for the S. Aureus), IV Gancyclovir (for possible CMV pneumonitis) and IV Amphotericin B and IV Septra (prophylactic dose).
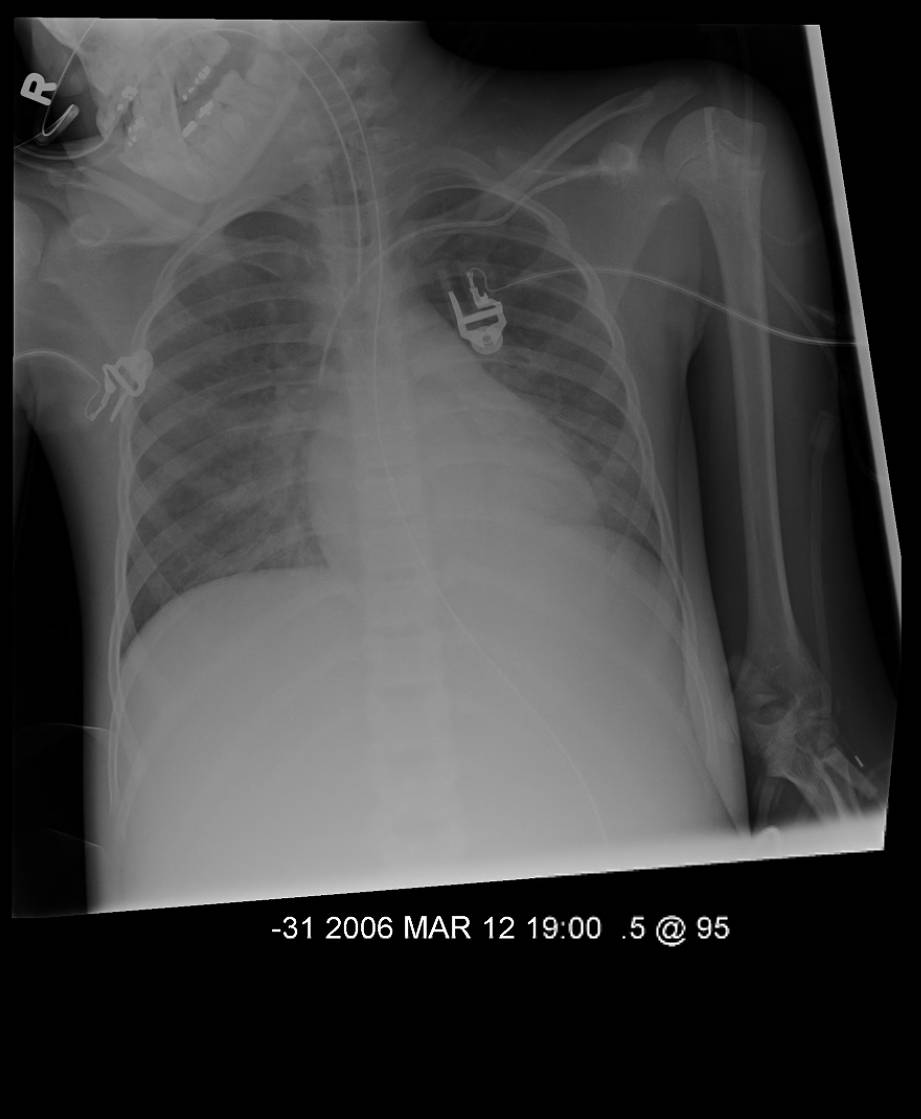
The respiratory status remained stable until Day 15 at which point she required increased ventilatory pressures (peak inspiratory pressure of 33 cm H20 and a PEEP of 12 cm H2O) and a FiO2 of 0.50. Her arterial blood gas was: pH 7.27; pAO2 73.5; pCO2 53.4; A-a gradient of 255.
A chest xray was obtained on Day 15
What is your interpretation?
figure 2