THERAPY FOR BOOP
–
PREDNISONE 1 mg.kg for at least 1 to 3 months, then possibly taper to
10 to 20 mg/day for a total of one year.
–
Relapse is frequent with shorter courses.
STEROID
NON-RESPONDERS:
– May respond to Cyclophosphamide
– Death in 5% (overall, 25% of non-responders)
– Poor prognostic factors (in adults) include an inderlying condition
(such as Connective Tissue Disease or Drug Therapy), widespread Interstitial
Opacities on CXR.
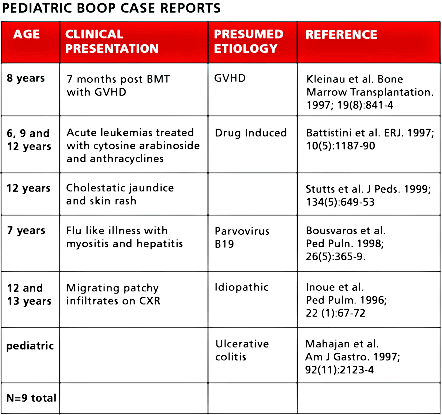
If one looks at the literature of bronchiolitis obliterans in children, there are probably also multiple cases of BOOP mixed in with the "constrictive" type of bronchiolitis obliterans.
The small amount of pediatric literature on BOOP, and our own center experience with BOOP, does not support the good prognostic, steroid responsive picture associated with this disease in adults.
After reviewing the literature, lets get back to our case.
Did
we identify an etiology for this young girl's BOOP?
NO:
– no inectious agent identified
– no rheumatological disease identified
– no nasty drugs identified
– no immunodeficiency identified
– post infectious seems to fit the clinical picture or early autoimmune
disease or idiopathic
How should we treat her? CONTINUE STEROIDS? TRY WEANING? Other antimetabolite drugs like cyclophosphamide?
WOULD ANYONE CARE TO OFFER A DIFFERENTIAL DIAGNOSIS AT THIS POINT
What
is her prognosis? We do not have enough knowledge to speculate. All we
can do is hope for the best!
